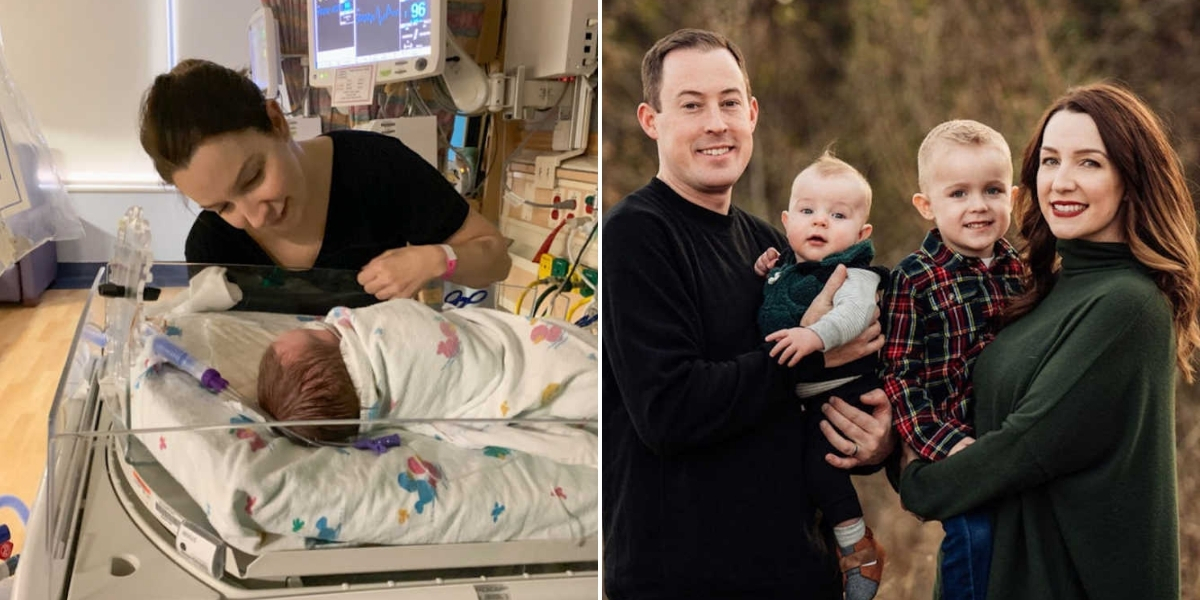
As a first-time mother in 2015, I was determined to breastfeed, and my biggest goal was to make it a full year nursing my son. I even took a “Breastfeeding 101” class at the hospital where I planned to give birth, hoping it would prepare me. But even that didn’t fully equip me for the challenges I would eventually face on my nursing journey.
My older son arrived in March 2015 after an emergency cesarean. I had been induced the day before and only progressed very slowly through the night. As contractions intensified, my baby didn’t respond well, and the nurses placed an oxygen mask on me while carefully watching his stats. When his heart rate suddenly dropped and he went into fetal distress, my OB/GYN rushed over from her office and told me I needed an immediate c-section. His heart rate had stayed dangerously low for too long, and he needed to be delivered right away.

Being wheeled into the operating room felt like a blur. I remember staring up at the ceiling, praying and trying not to panic as the bright lights shined over me. My heart rate climbed so high the anesthesiologist repeatedly reminded me to breathe slowly and deeply. Within the hour, I was in recovery holding my baby boy — thankfully, perfectly healthy. Because of the c-section, my milk came in slower than usual, which is common. I nursed him every two hours, but he still wasn’t getting enough colostrum, so we supplemented with formula for a short time. Since he was full-term, donor milk wasn’t an option. Once we came home, those first two weeks were tough as he struggled with weight gain.
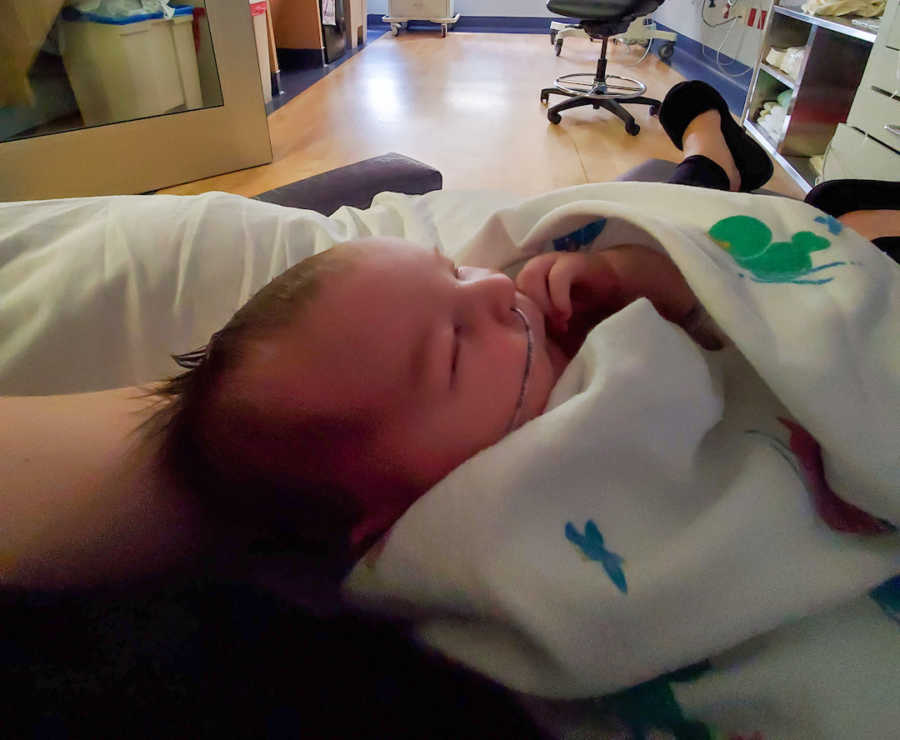
To make sure he received enough milk at every feeding, I pumped between nursing sessions and used a supplemental nursing system (SNS). My pumped milk went into a bottle with a tiny tube taped to my breast, so he could get milk both from me and through the tube. My husband often held the bottle upright so it would flow properly. Eventually, my son gained back his weight and didn’t need formula again. I kept pumping to build a freezer stash for a three-day trip we had planned when he was six weeks old. Waking at 3 or 4 a.m. to pump on top of caring for a newborn was exhausting, and I kept that routine going for over a month.

Soon, I found myself with an oversupply. My son breastfed exclusively and refused bottles, leaving my freezer full of milk I didn’t need. With no local milk banks in my area, I donated to two moms from an online breastfeeding support group whose babies needed extra milk and whose own supply was low. I felt proud not only to surpass my goal — nursing my son until he was 21 months old — but also to help other families.

Fast forward to July 2019, when I became pregnant with my second son. Wanting more support for a VBAC (vaginal birth after cesarean), I hired a doula. She told me about a local milk bank — Mother’s Milk Bank of North Texas (MMBNT), a nonprofit that supplies donor milk to premature and critically ill infants when their mothers’ milk isn’t available. After calling the hospital where I planned to deliver, I learned donor milk there was only for non-full-term babies.
After four days of prodromal labor and a full day of regular labor, I successfully delivered my second son vaginally — something I had prayed for. But my joy shattered when we learned he had severe meconium aspiration. He had inhaled his own stool sometime during labor, and although this can happen, his infection was unusually serious. He was immediately taken to the NICU, and we waited for hours just to see him.

He was placed on medications and ventilators to clear his lungs and help him breathe. That same night my colostrum came in, and by morning I began pumping since I couldn’t nurse him directly. Emotionally and physically drained, I still pumped faithfully every 2–3 hours.
On the second day, our world stopped. The neonatologist explained that our son wasn’t stabilizing, and his heart was working dangerously hard against the ventilator. She warned that he might need ECMO — a form of heart-lung bypass surgery. Our hospital didn’t have the machine, so plans were made to transfer him to Medical City Dallas Children’s Hospital, home to the highest-level NICU in our area.

He stabilized just enough to travel. I was discharged early so I could go with my husband as we followed the ambulance through the dark early-morning roads. Hours passed before a doctor finally updated us. Our baby was still critical but improving — and, thankfully, did not require ECMO. After scrubbing in, we were finally allowed to see him. Wires covered his body, and even gentle touch overstimulated him, so all I could do was softly rub his forehead and sing.
The NICU had a dedicated lactation room, and I was grateful for a quiet place to pump and breathe for a few minutes at a time. I pumped at home every 2–3 hours as well, bringing milk back to the hospital for his feeding tube. I often produced more than he needed, so the extra stayed in a small fridge in his room. Each day, we drove an hour each way to the hospital, since the NICU didn’t have room for me to stay overnight.

Our families stepped in to help care for our older son so we could focus on the baby. Gradually, he improved and began coming off machines. After weeks, we finally got to hold him — a moment I will never forget. Holding him while he was still connected to tubes was overwhelming, and the constant alarms kept me on edge, but the joy outweighed the fear.
Two weeks later, we tried nursing, but he still needed to relearn how to breathe and swallow without aspirating. Eventually, he moved from critical care to another floor for recovering babies. He continued tube feedings every three hours while we slowly introduced bottles of my milk. Progress was slow but hopeful.

Doctors were cautious about removing the feeding tube until he could reliably breastfeed or bottle-feed. With approval from the doctor and OT, I tried nursing again — and this time, he improved little by little. Eventually, his tube was removed. To be discharged, he needed to gain a specific amount by nursing alone, so I stayed at the hospital around the clock for nearly three days, feeding on cue and surviving on almost no sleep. Still, caring for him nonstop felt like such a gift after weeks of separation.

Finally, we brought him home — an exclusively breastfed, full-term NICU graduate, which is incredibly rare. I continued nursing and pumping occasionally, and soon our freezer overflowed again. I contacted the milk bank, completed the health screening, and had my blood drawn at no cost. A few weeks later, I was officially approved as a donor.

Months later, I dropped off my first donation at the same hospital where I’d delivered him — an emotional full-circle moment. In April 2020, MMBNT sent me a certificate: I had donated 787 ounces — over six gallons! I kept pumping and storing milk, unsure whether I would donate again.
By the next April, my freezer was once again packed. Knowing my son wouldn’t use it, I made one final donation. My husband drove our family more than an hour to Fort Worth so I could deliver the milk. Because of COVID restrictions, I couldn’t tour the building, but standing outside for a few photos still felt special.
Just before Mother’s Day, I received an email thanking me for donating another 227 ounces — nearly two more gallons — bringing my total to 1,014 ounces. Almost eight gallons of milk went to fragile babies who desperately needed it. Writing this brings tears to my eyes, remembering every hurdle I faced to breastfeed both my boys — something that seems like it should come naturally.
My sons will always be my greatest blessings, but being able to donate so much milk and support other families is an honor I’ll cherish forever. If you’re a mom with extra breastmilk — or the desire to pump specifically to donate — I encourage you to contact your local milk bank. And if you live in Texas, texasmilkbank.org is an amazing place to start.