Growing up, I often said I would “die young.” Over the years, I’ve learned that “young” isn’t a fixed age—it’s a moving target, and life has a way of humbling you when you least expect it.
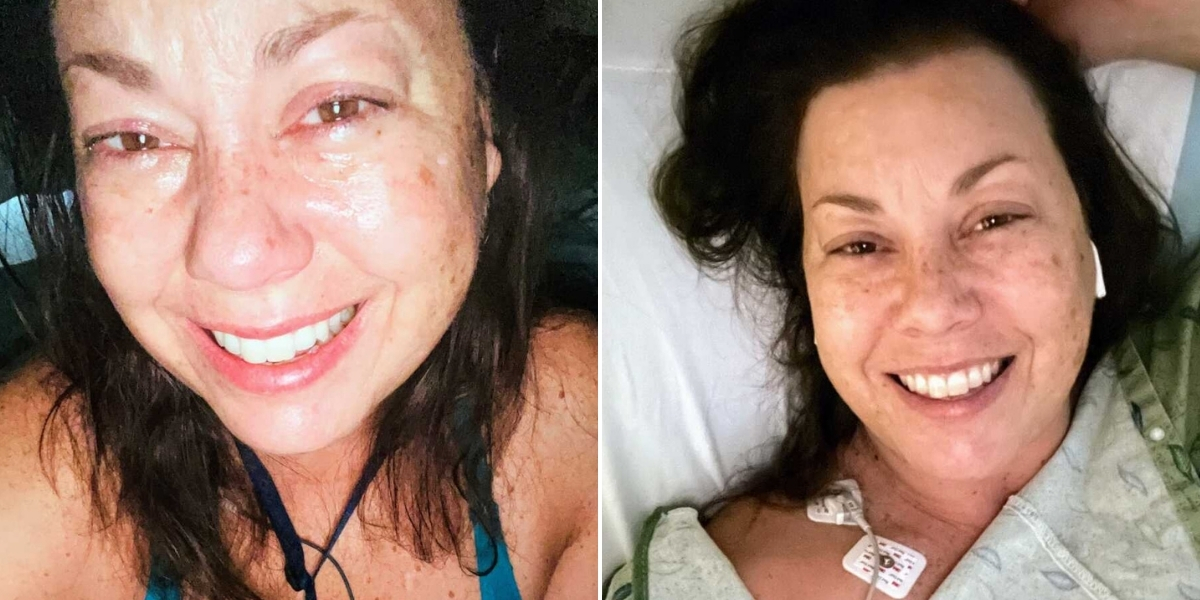
At 43 years “young,” I discovered just how fragile life really is. Eight days before my 43-and-a-half birthday, on a hot, sunny Friday morning in Arizona, my life took an unexpected turn. My morning began as usual—teeth brushed, face washed, pets fed. I locked the back door after my husband left for work and stepped through the kitchen. Suddenly, the right side of my body felt heavy. My knee buckled, walking became a struggle, and a lightheadedness, like a dizzy high, overtook me. Fear surged, but deep down, I found a calm I would soon learn was essential for the days ahead.

That morning, I had plans—a friend from animal rescue was coming to clean couches and rugs, and I also had a telephonic meeting with my ACLU team about a large project. I pushed through, determined to honor both commitments. I called my doctor, but he wasn’t available. The staff advised me to go to the ER because of possible stroke symptoms. My face wasn’t drooping, my speech was clear—I thought maybe it was just my back or neck. Still, I called my sister-in-law, a doctor, and she insisted I go immediately. Both my arm and leg were affected, and she was very concerned.
I drove to the nearest hospital, located in a rural area not fully equipped for major emergencies. I waited in the lobby for nearly three hours, convincing myself that I must be okay. Exhaustion settled over me, but I felt I was exactly where I needed to be. When admitted to the ER, I met the weary but compassionate staff. COVID had slowed care, but I stayed positive. While waiting for my brain CT scan, a man was rushed into the curtained area beside mine in critical condition. I watched as life-saving measures were performed. Intubated, fighting for survival, he needed the care more than I did—or so I thought.
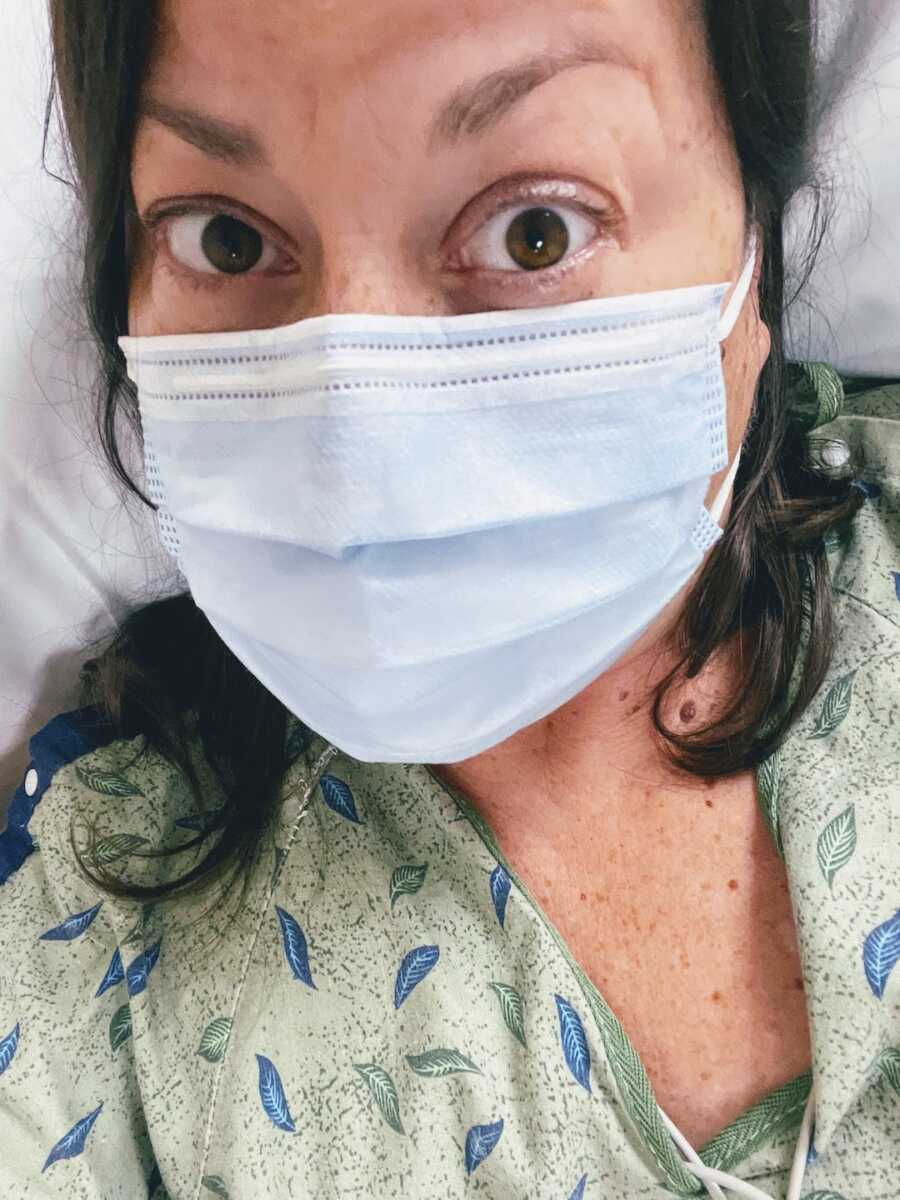
Later, I was wheeled for the CT scan. I joked with the tech that I didn’t think I’d return to my ER room afterward. He assured me I would. On return, I found both sides of the ER room filled with equipment to save the man’s life. My stretcher was positioned in the hallway for over an hour. Outside, a monsoon had turned Arizona roads dangerous; paramedics brought in accident victims. Observing the chaos kept my mind from darker thoughts. At some point, a doctor gently shook my shoulder to wake me, checking on me before reassuring that I’d soon return to the ER room.
My CT scan showed no major clot or blockage. The ER doctor said we were on “team migraine” for the night, with an echocardiogram and MRI scheduled for the next morning. I was moved to the ICU, partly because no other beds were available and partly to ensure constant monitoring. Alone in the sterile ICU room, I felt a wave of childhood memories of my tonsillectomy—how my mother would stay by my side, tickling my hands to comfort me. Here, my nurse became my sole human connection, offering care, reassurance, and kindness. The only decoration was the covers on the large fluorescent lights above my bed, featuring butterflies against a sky-blue backdrop—small signs of life in a sterile environment.
Alone, I cried. Even without answers, I knew this was far more serious than a migraine. Saturday morning brought my MRI. Fear hadn’t fully set in yet; I mentally prepared for what might come. By 2 p.m., without any results or IV medication, I considered self-discharging, thinking perhaps I was truly just on “team migraine.” Then, at 4 p.m., everything changed. The young doctor entered, sat beside me, and quietly said, “Your MRI came back—you’ve had a small-vessel stroke.” Time seemed to freeze. My soul felt winded. I had a stroke. I was in the ICU. Now what?
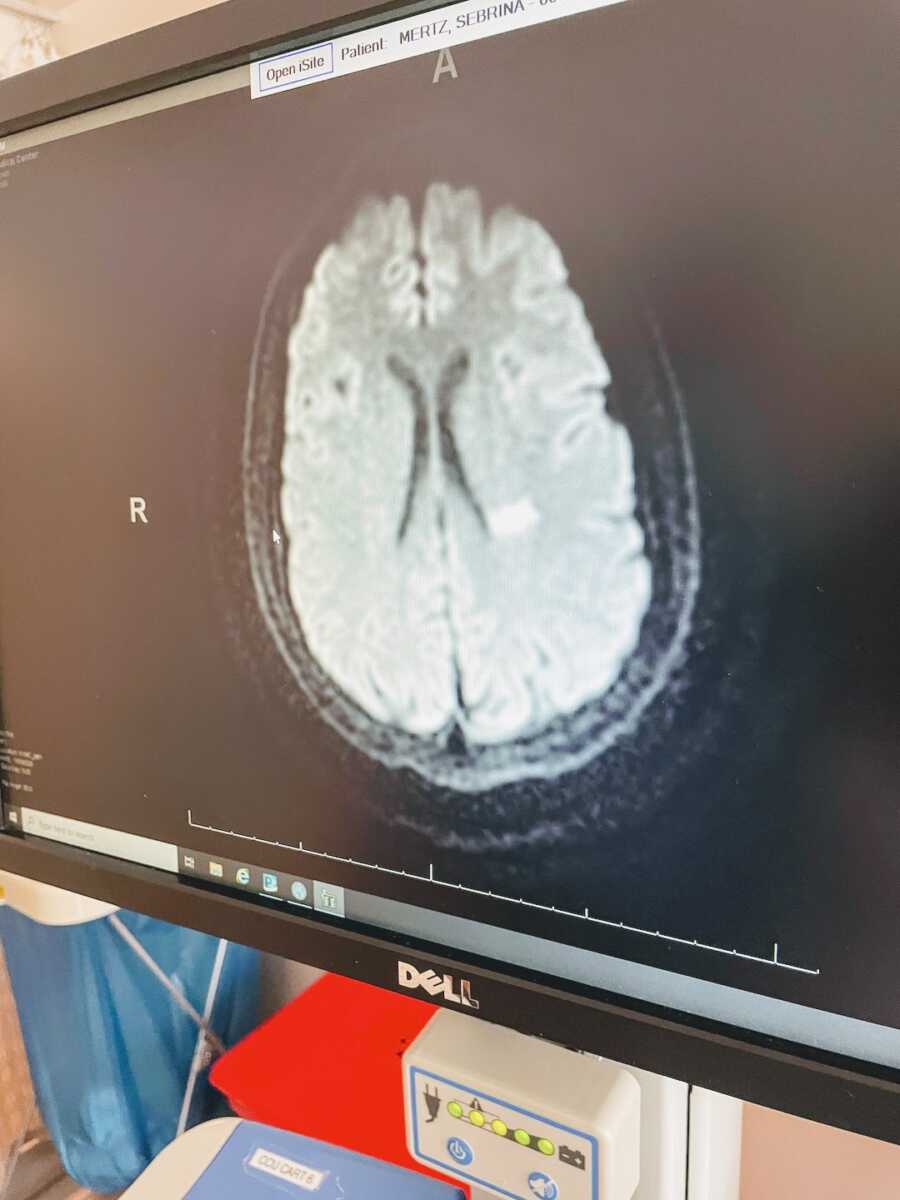
He showed me the MRI: a small, rectangular white space on the left side of my brain, just below the ear—a permanent mark, like a tattoo of the stroke. I was instructed to remain for another 24 hours for observation and blood thinners. I let go of any thought of leaving, called my parents, and cried silently into my hospital pillow.
Recovery became my mission. With the guidance of a neuro-therapist recommended by a friend, I worked tirelessly for two weeks to regain strength in my right side. I recovered physically faster than I expected, but mentally, the stroke left its mark. Mood swings, sudden tears, and an instant temper became part of my reality. During a particularly emotional physical therapy session, I laughed for the first time in days, joking with my mom that I was not a “Superstar,” but a “stroke star.” Throughout, I was surrounded by love, support, and encouragement from family, friends, and my online community. Sharing my story publicly, as I had done during my COVID battles in 2020, became my outlet. Writing about it helped me heal and raise awareness.

The “why” lingered—why this stroke, why now? My neurologist at Barrow’s ordered extensive lab tests to rule out clotting disorders. Known as a “tough stick,” I endured 16 tubes of blood drawn in early September 2021. Joking with the PICC line nursing team that it was a “date with a team of vampires,” we laughed together. Despite anxiety, I held onto humor and kindness.
On September 29, 2021, my life gained clarity: I was diagnosed with a rare blood clotting disorder, APS (antiphospholipid syndrome). The stroke was caused by abnormal antibodies produced by my immune system, likely triggered by COVID. The past year of illness and challenges came full circle. COVID had been the gift that kept on giving—but it also taught me the profound value of life. Each day, each moment, is a gift.
I often tell my criminal defense clients, “It’s not forever, it’s just for now,” to shift perspective and overcome hardship. Today, that mantra is mine as well. Life is fragile, unpredictable, and deeply precious—and I’ve learned to embrace every single moment, grateful for the journey, the recovery, and the love surrounding me.