Kristy and I both came to the same realization in the summer of 2015. Our boys, Oliver and Micah, were 6 and 4, and for years we’d held firm to our “two is enough” pact. But deep down, our family felt unfinished. After many late-night conversations, we agreed to try for one more child. A few months later, we were overjoyed to learn Kristy was pregnant, and the quiet dream we’d shared started to take shape.
Because she worked as a labor and delivery nurse at a major hospital, Kristy kept an informal eye on things. I joined her at the first official ultrasound, where we learned we were having a baby girl. “You’re 24 weeks, right?” the tech asked casually. “No, 21 and 2,” Kristy answered confidently. The tech frowned. “That’s odd. Her head is measuring 24.” Thinking it was just an angle, she brought in her supervisor. Kristy joked our daughter must be inheriting Micah’s big head. But the appointment ended with referrals to high-risk neonatology for two concerning findings: ventriculomegaly and echogenic bowel.
Things grew complicated quickly. The first specialist had trouble visualizing a kidney — it was there, just hard to see — and thought the skull looked irregular. He ordered both a fetal MRI and an amniocentesis. Our nerves rose with each appointment. In an effort to comfort us, a doctor Kristy had worked with for years said, “God gives special babies to special people.” I understood his intent, but the words landed heavily and would echo in my mind for months.
We sought a second opinion from a highly respected physician. Because of an important work accreditation, I couldn’t make the appointment — a decision I regret deeply. During my lunch break, Kristy called, barely coherent. “Dr. H is 90% sure the baby has syndromic craniosynostosis. Don’t Google it.” I left immediately and cleared my schedule. The amnio later confirmed Pfeiffer Syndrome — an FGFR2 mutation that causes skull plates to fuse prematurely. The doctor had been right.
The next day, Kristy’s dear friend Sarah came over. We sat together at the dining room table — numb, scared, and trying to understand what this meant. Sarah gently said, “Of all the couples I know, you two can handle this. Hadley will be so lucky to have you.” Her words steadied me. I shifted into problem-solving mode, while Kristy wrestled with anxiety and began losing weight. We unknowingly fell into a rhythm that has carried us ever since: when one of us faltered, the other grew strong.
A local craniofacial team walked us through what to expect. Hadley would likely need cranial vault reconstruction (CVR), a frontal orbital advancement (FOA), and possibly later, midface advancement and jaw surgery. There wasn’t a strict algorithm — every child’s path is different — but at least there was a roadmap.
Hadley arrived on June 2, 2016, via scheduled C-section after two breech weeks. Sarah and Alyssa, both close nurse friends, cared for Kristy that day. When Sarah confirmed Kristy was actually dilated — and that Hadley had flipped head-down — the nurses laughed. I chewed a peppermint, fighting a quiet unease. The surgery went smoothly, and when they placed Hadley in our arms, she was delicate, beautiful, and somehow still unfamiliar. Yet our love for her was immediate.
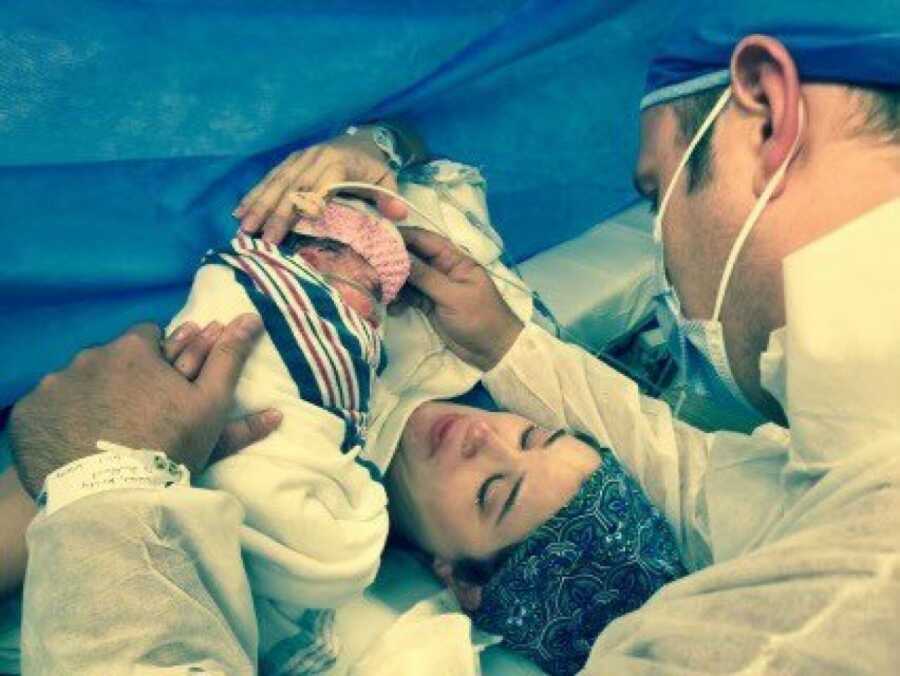
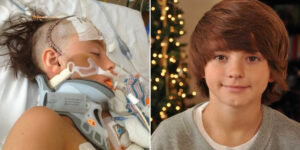
Her skull was domed due to fused sagittal and coronal sutures — brachycephaly. But her vitals were strong. After four cautious days in the NICU, we took her home and soaked in a precious honeymoon period — until mid-July, when her eye bulged for the first time.
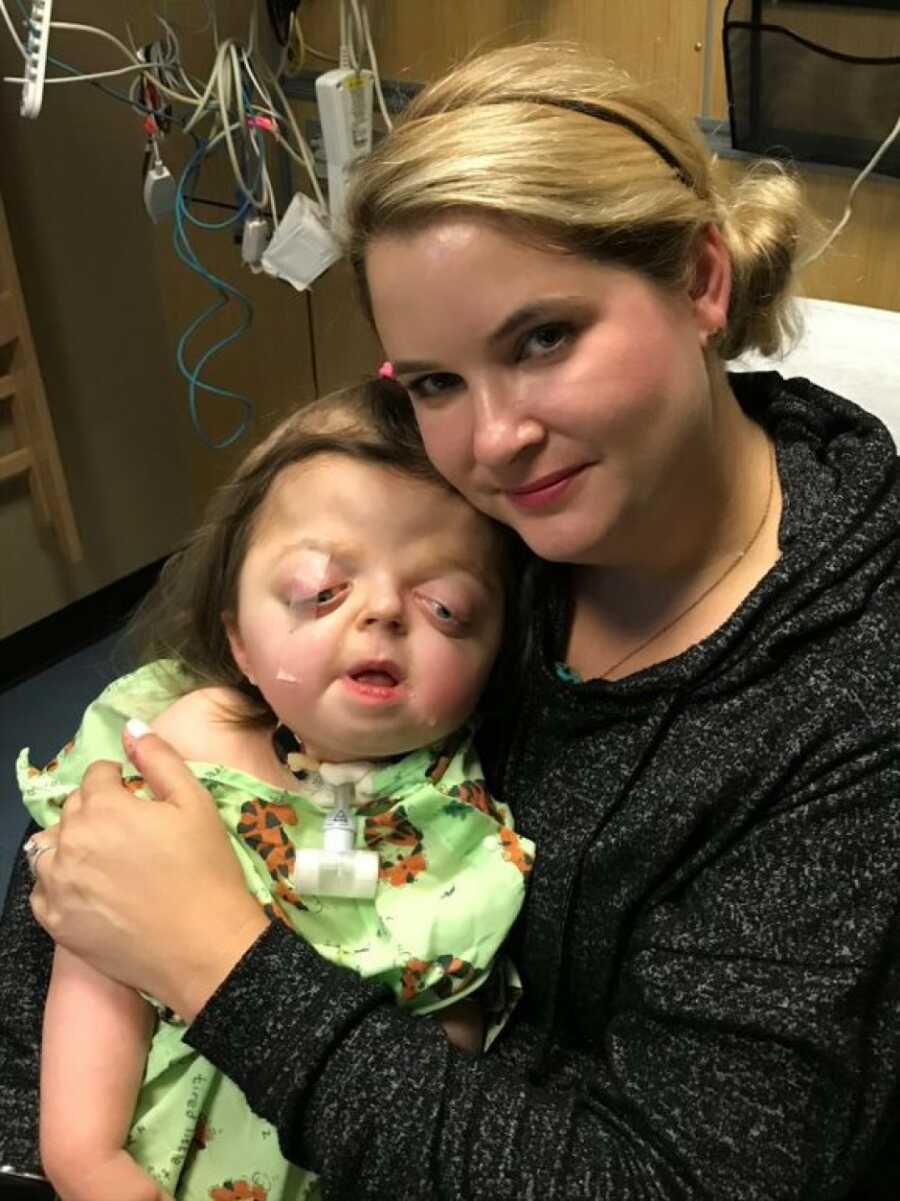
Children with Pfeiffer Syndrome often have a recessed midface, leading to proptosis. With less bone protection, coughing or straining can cause the eye to shift forward. For months we battled these episodes, gently guiding her eyelid back over. Surgery had already been discussed, but when Hadley’s right eye became stuck beyond the lid on September 16, everything changed. Somewhere between birth and three months, she had developed severe hydrocephalus. She urgently needed surgery to relieve pressure. Over nine long hours, surgeons performed CVR, FOA, and placed a shunt while Kristy and I waited alone.
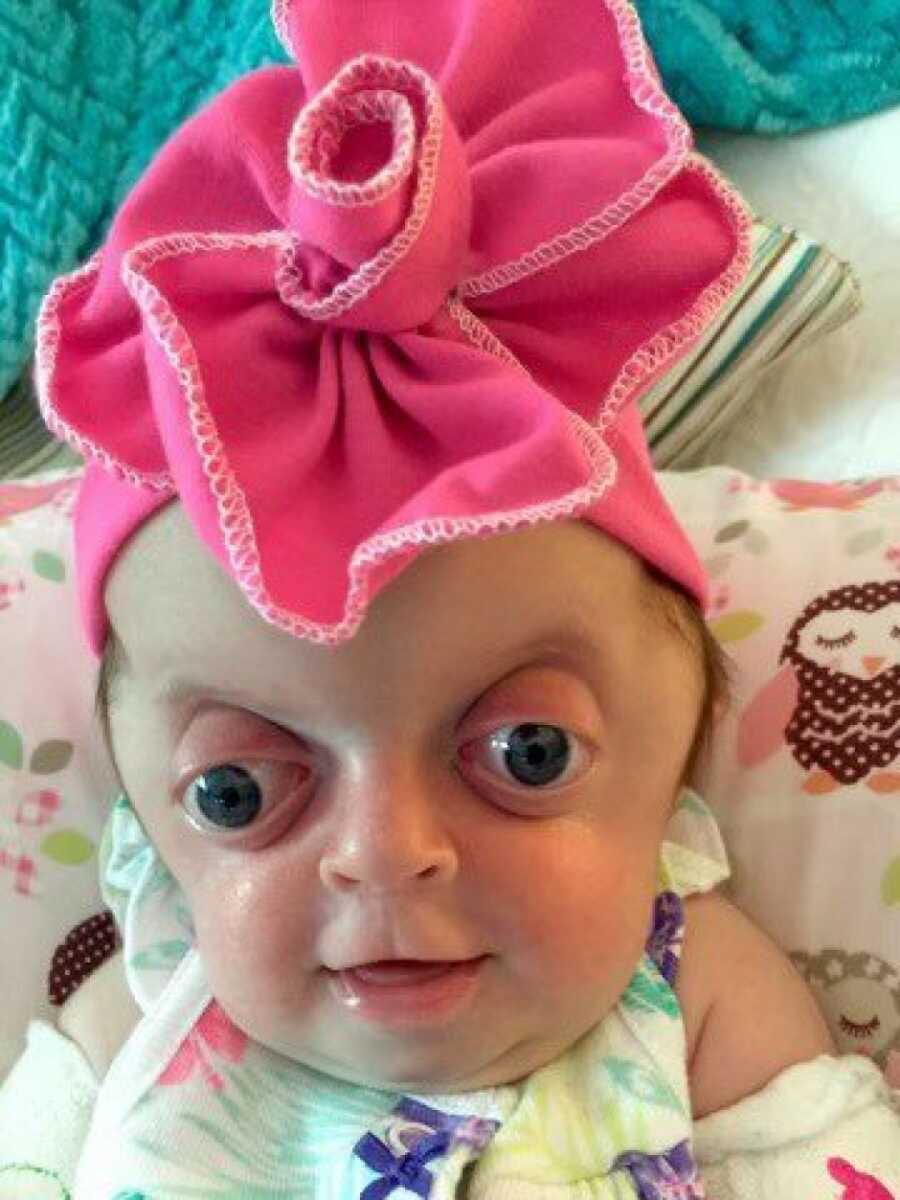
By every medical standard, surgery was a success — her skull looked incredible. But two days later she developed a pseudomonas infection. After ten grueling hospital days, doctors had no choice but to remove her right eye when she was four months old. Even knowing the risks, nothing prepared us for this detour. Our surgeon said that in over 800 cases, this had never happened before. Being the rare outlier within an already rare diagnosis felt brutally isolating.
Slowly, our family adapted. Balancing care for Hadley with parenting our boys took time and patience. My parents stepped in constantly, bridging gaps we couldn’t. After a poor sleep study and increasing dependence on oxygen, we decided a tracheostomy would give Hadley the best chance. The boys spent the summer in Minnesota with my parents while we learned new medical skills and watched Hadley heal.

The following summer, we began traveling to Boston Children’s Hospital. Flying with medical equipment was exhausting and always invited stares. Once, our oxygen concentrator died 15 minutes before landing. Hadley’s levels plummeted. I grabbed a green tank, rigged the tubing, and prayed. Moments like that taught us that instincts and improvisation would often become our greatest allies.
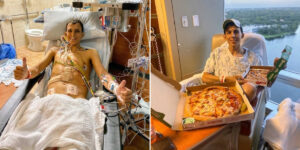
Hadley eventually underwent a Chiari decompression to relieve pressure at the base of her brainstem. Two days later, she began breathing room air — and held her oxygen beautifully. That small miracle brought enormous relief and hope.
For a while, life felt like progress. She grew stronger, needed oxygen only occasionally, and started using a Passy Muir valve. Then came the garage sale morning. Kristy was outside negotiating deals. I was inside with Hadley when she suddenly stopped breathing. Even after suctioning, her levels sank. I changed her trach, added oxygen, and called for Kristy. Seconds later, we were racing to the ER.

In triage, Kristy insisted we be seen immediately. Moments after we reached the room, Hadley’s leg twitched — then the full seizure hit. For what felt like forever, we stood helplessly as doctors worked to save our coding daughter. Eventually, they stabilized her. Tests revealed dangerously high CO2 levels, leaving her too exhausted to breathe properly. She bounced back — amazingly — but now needed a nighttime ventilator. Our pulmonologist found a model that monitored gas levels; humor, however dark, carried us through. “If she has to have a vent,” I joked, “it might as well be sexy.”
The ventilator completed our “bionic” girl. Life steadied into something imperfect but deeply ours. Development came slowly — and neurology later added cerebral palsy to her diagnoses — yet none of it defined her. Hadley was still Hadley.

Through five years of surgeries, scares, and small victories, our marriage stretched and strengthened. Our boys grew incredibly compassionate, loving their sister fiercely and adapting with resilience. I’m endlessly grateful for them.

We’ve built friendships through shared experiences and found community through organizations like the Children’s Craniofacial Association. Social media became a space where I could share honestly — not to seek pity, but to normalize medically complex families and celebrate our children. On Hadley’s pages, I try to balance humor, vulnerability, and love. Creating those memories gives us purpose — and Hadley is the perfect comedic partner.
Hadley’s life isn’t what we pictured when we decided our family felt incomplete. But she is exactly what our hearts needed. We strive to give her every opportunity to grow, while recognizing the light she already brings. She is joyful, deeply loved, and absolutely worthy. If I could change anything, it would be missing that one early appointment — I made the next hundred before I stopped counting. We can’t always erase mistakes, but we can always show up for the people we love.