I am honestly not sure where my story truly begins. I can’t pinpoint an exact moment when my symptoms first appeared. I can only look back to my early teenage years and recognize what were likely the first quiet signs that something in my body wasn’t quite right.
As a teenager, I was a competitive gymnast. Even then, I remember feeling more easily fatigued than my teammates. My mom took me to the doctor to have my iron levels and thyroid checked, but I was told everything looked normal and that I was healthy. When I was 15, I suffered a back injury that abruptly ended my gymnastics career. It should have healed quickly, but instead the inflammation, pain, and violent muscle spasms lingered for years. It felt as though my body was reacting far beyond what the injury warranted.
Eventually, the pain became somewhat manageable, but it never fully disappeared. At 15, my complaints were not taken seriously. I was repeatedly told it shouldn’t hurt that badly and that there was nothing more to be done beyond pain medications, muscle relaxers, and repeated steroid injections. Imagine being a 15-year-old and feeling like the medical world had already given up on you.

In college, the neck and back pain followed me, along with relentless exhaustion. I missed classes regularly because I physically could not get out of bed. When I sought help from the campus physician, he concluded I was depressed and prescribed antidepressants. Since I wasn’t actually depressed, the medication triggered manic-like episodes. Despite not being qualified to diagnose me, he decided I must be bipolar.
Over the next two years, I was prescribed a rotating list of antidepressants, mood stabilizers, and antipsychotics. The inappropriate medication combinations caused auditory hallucinations and led to attempts at self-harm. After two psychiatric hospitalizations, a qualified psychiatrist finally evaluated me and determined I was not bipolar. He encouraged me to seek a different primary care physician to explore possible physical causes for my exhaustion. By that point, the fatigue and medication side effects had forced me to drop out of college entirely.
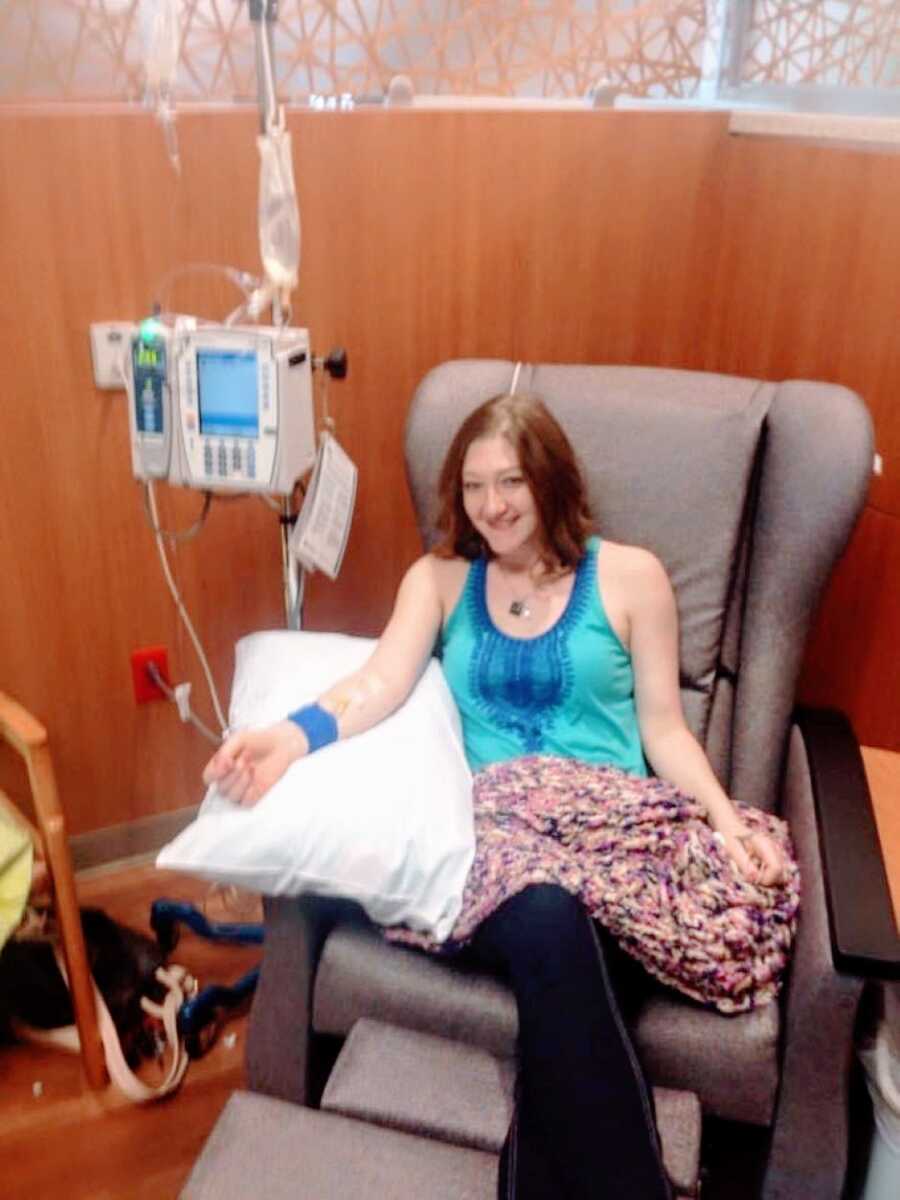
Over the next several years, I saw countless doctors for symptoms that seemed unrelated on the surface. To them, I was just a healthy-looking young woman in her twenties who complained too much. I was dismissed again and again. In 2006, I had wrist surgery to remove a painful cyst, but two months later the pain and inflammation were still severe, and I was placed on steroids. At my follow-up appointment, I told the surgeon that while on steroids, I felt better than I had in years. I had energy, I slept better, and I wasn’t constantly in pain. For a supposedly healthy person, that reaction wasn’t normal.
Concerned, he ordered lab work that came back abnormal, indicating something was indeed wrong. For the first time, there was proof. I wasn’t crazy—or so I thought.
My primary care physician ran additional labs with the same abnormal results and referred me to the only rheumatologist within several hours’ drive. I had my first appointment the day after my 24th birthday in February 2007. I wish I could say that appointment brought answers, but it was only the beginning. After nearly a year of repeated labs, tracking symptoms, doing my own research, and begging to be heard, I was finally diagnosed with Systemic Lupus Erythematosus. I was able to start medication to manage my symptoms and slow disease progression.
Unfortunately, my then-husband and I were relocating from Abilene, Texas to College Station. I scheduled an appointment with the only rheumatologist available there to continue care. Despite receiving my medical records, the new doctor ordered more labs and then told me what I had heard since I was 15: there was nothing wrong and I didn’t need to return. I was devastated. My husband echoed the same belief, often telling me I was weak and lazy. I managed to see another rheumatologist briefly, but she believed I wasn’t sick enough to warrant treatment.
For the next four years, I managed my symptoms as best I could. I was fortunate to have a wonderful internist who truly listened and addressed issues as they arose. During that time, I got divorced, remarried my high school sweetheart in 2012, and moved to a new town. Life felt full and hopeful. I was in a loving, supportive marriage and physically felt better than I had in years. I stayed home, cared for our house, animals, and my husband, and felt genuinely content.

In September 2012, I decided to start the P90X workout program. It was challenging, but I loved it—at first. About two months in, the workouts became harder instead of easier. Getting out of bed became a daily struggle. I started feeling nauseated during workouts, my muscle soreness was extreme, and when I began vomiting during exercise, I finally stopped.
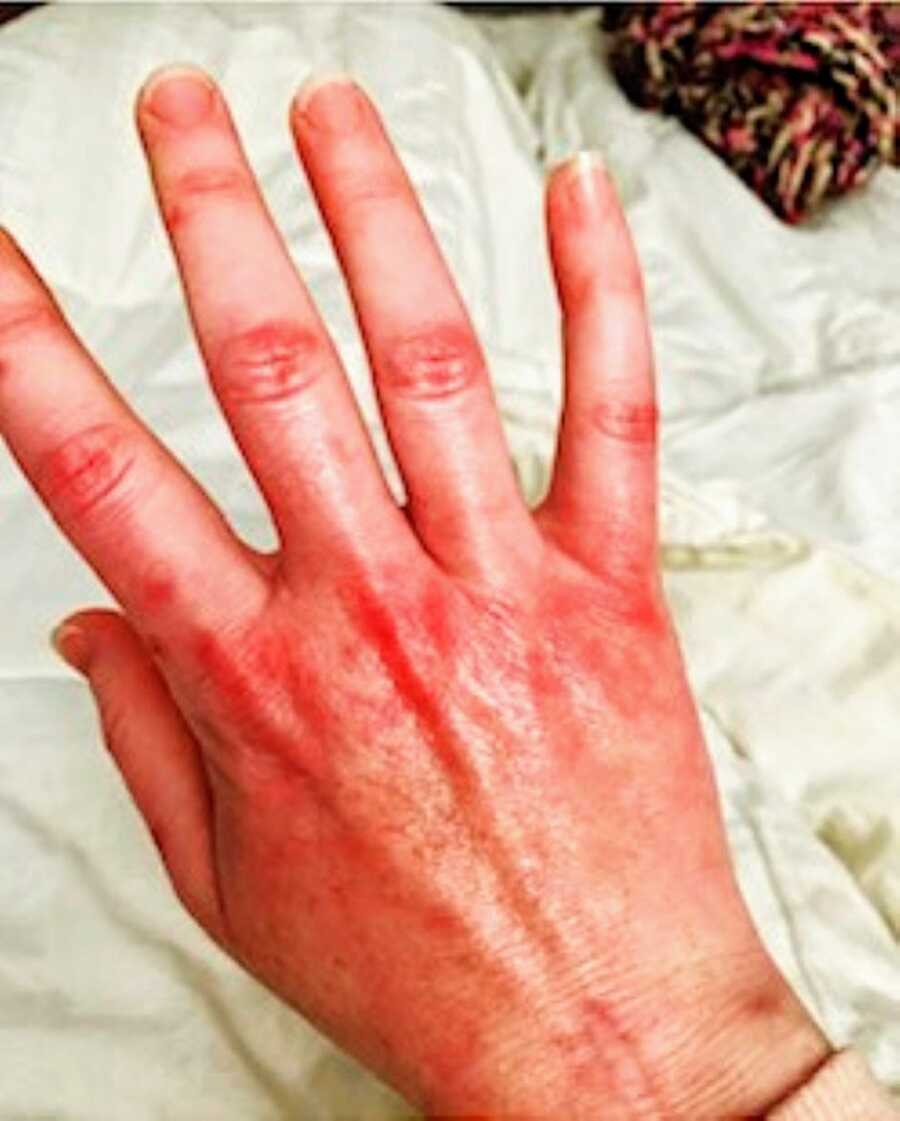
My PCP took my concerns seriously and ran tests, which revealed I had overstressed my kidneys. A few weeks later, I landed in the ER with severe chest pain and pleurisy. Over the next year and a half, I went from a functioning, relatively healthy 28-year-old to a shell of myself. I was on steroids every few months for recurrent pleurisy. My hands became so painful and stiff that basic daily tasks were difficult. My doctor suggested chemotherapy medications, but that meant putting my lifelong dream of having a baby on hold.
Then the cognitive issues began. I struggled to hold conversations, slurred my speech, lost words, and got lost driving familiar routes. My doctor finally explained that pregnancy was too dangerous in my current state and that controlling my lupus was the only chance I had at becoming a mother. With that realization, I began Methotrexate, a chemotherapy immune suppressant.
With autoimmune disease, the immune system attacks healthy tissue instead of invaders. Immune suppressants are used to slow that attack, but they leave you dangerously vulnerable to infections. Even minor illnesses can become life-threatening. When infections occur, medications must be stopped—allowing the immune system to surge again.
In 2014, after multiple infections and time off medication, I developed pericarditis, a serious inflammation of the heart. My disease had progressed beyond what my PCP could manage. Despite my fear from past experiences, I was referred to a rheumatologist. My doctor reassured me this time would be different.
That’s when I began seeing Dr. Olga. Under her care, I received IV therapies and oral medications. In 2016, I was finally healthy enough to try for a baby. I became pregnant in April, but after a devastating emotional journey, I miscarried in June—likely twins. A previous history of three miscarriages had already led to a diagnosis of a lupus-related clotting disorder. I became pregnant again in September and miscarried in October.
In December, I saw two lines once more. This baby held on. The pregnancy was filled with constant monitoring, bedrest, blood thinners, weekly ultrasounds, labs, and overwhelming fear. Both my baby and I were high risk. On August 11, 2017, I was induced and gave birth to Faith—a perfectly healthy 6 lb 13 oz baby girl.


I remained in remission until Faith was just over a year old. Since then, despite aggressive treatment, my disease has become uncontrolled. Being severely immune compromised during the pandemic has been terrifying. In 2019, rheumatoid arthritis was added to my diagnoses. Abnormal blood work suggests possible bone marrow involvement. In June 2021, I underwent a hysterectomy due to painful fibroids and the life-threatening risk pregnancy would pose.

My health journey is far from over. I live with worsening exhaustion, chronic pain, recurrent infections, hair loss, and uncertainty. Some days I feel unstoppable. Other days I feel like a burden. Often, the only thing that gets me out of bed is my daughter who needs her mom. Without my family and friends, I could not do this.

If I could offer advice, it would be this: don’t give up. Advocate for yourself. Find doctors who listen. Build a support system. If someone you love is chronically ill, believe them. They are not weak, lazy, or exaggerating. Every day is a battle.
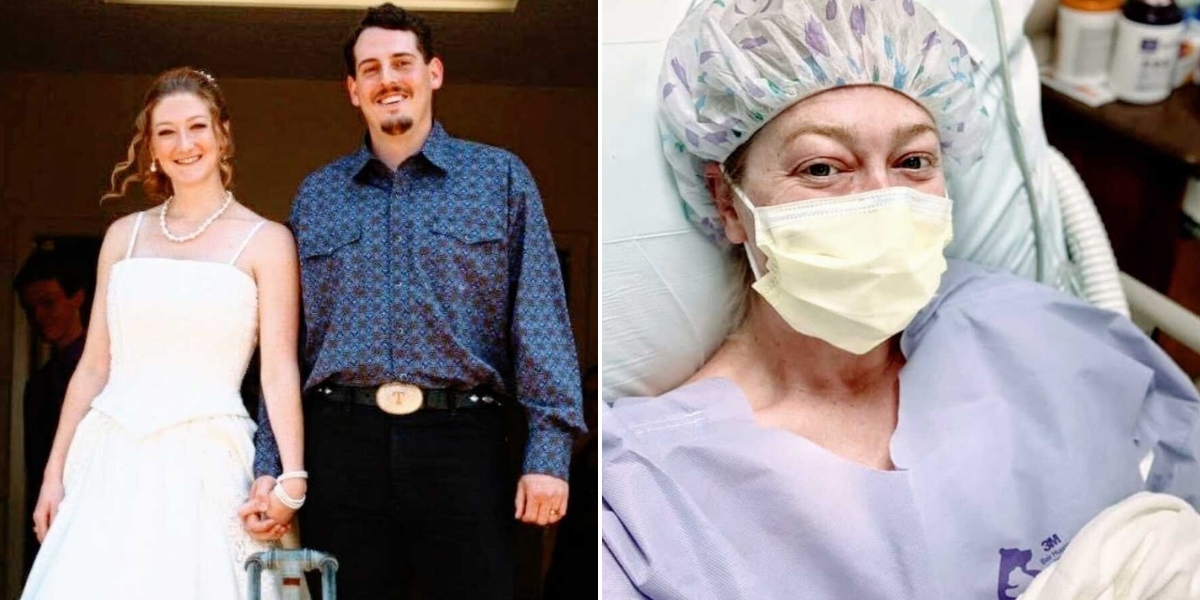
Do not judge someone by their appearance. In photos, I look happy and healthy. Behind some of those smiles, I was losing my babies and barely surviving. But I am still here. And that is the point.