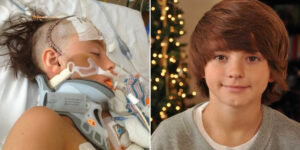
My family has a long history with a rare hereditary disease—Familial Adenomatous Polyposis (FAP). My mother and grandfather both lived with this condition, and from birth, my parents knew there was a 50/50 chance I would inherit it. FAP is caused by a genetic mutation that leads to hundreds or even thousands of precancerous polyps in the colon, which will inevitably become cancerous without intervention. The standard treatment is to remove the colon before cancer develops, often requiring an ileostomy, temporary or permanent. These polyps can also appear elsewhere along the gastrointestinal tract, and FAP can lead to additional health challenges, including Desmoid tumors, abnormal bone growths, extra teeth, and an increased risk for other cancers.

By age eight, I started experiencing chronic abdominal pain. Insurance requirements meant I needed a referral from my pediatrician to see a GI specialist, but my PCP dismissed my symptoms, calling me a “whiny child.” This delayed my care. My parents quickly switched insurance plans so I could be evaluated by a pediatric gastroenterologist. During my first appointment, my doctor ordered immediate medical and genetic testing due to my family history. The results revealed the source of my abdominal pain: my stomach was pre-ulcerous from stress, I had precancerous colon polyps, and, as suspected, I had inherited FAP.
By age nine, my precancerous polyps were beginning to turn cancerous, and I needed my colon removed. The plan was a two-step surgery: colon removal with a temporary ileostomy, followed months later by a reversal into a J-pouch. I was familiar with ostomies because both my mother and grandfather had them, so this part of the diagnosis was initially manageable.
My first surgery at the local children’s hospital, however, quickly became life-threatening. Weeks after the procedure, my incision became infected and had to be reopened and packed in the ER—without anesthesia or effective pain management—one of the most excruciating experiences of my life. Soon after, my small intestine twisted, cutting off blood circulation to a portion of it. My parents rushed me to the ER, but the first doctor dismissed my symptoms, calling me “just a whiny child” and sent me home with pain medication. The next morning, a different doctor conducted further tests, discovered the twisted intestine, and scheduled emergency surgery. I was told it was a miracle I had survived the night. Unfortunately, the lack of blood flow caused part of my small intestine to die, including the J-pouch, leading to two additional surgeries over the next year to remove adhesions and attempt a Straight Pull-Through for ostomy reversal.
Despite these efforts, my initial surgeon did not complete the ostomy reversal, leaving me with an ostomy for six years before finding another surgeon. The removal of my colon and part of my small intestine resulted in another rare condition—Short Bowel Syndrome (SBS), which causes severe diarrhea, dehydration, and malnutrition from nutrient malabsorption. Some individuals with SBS require artificial nutrition, and I faced the daily challenges of this condition for years.
The medical trauma left me with PTSD, and I repressed many memories as a coping mechanism. I do remember one kind nurse at the children’s hospital who I bonded with; my parents and I even attended his wedding. During one hospitalization, I formed a friendship with the child in my room, which lasted for years. In another stay, I briefly met Reba McEntire and the cast of Mighty Ducks for a hospital contest, but at the time, I was too unwell to feel excited. Simple procedures, even blood draws, became torturous due to my PTSD. I often had to be restrained for treatments, and I developed a deep mistrust of doctors. Middle school was particularly difficult; combined with bullying, my ostomy, and medical PTSD, I struggled with depression and anger, even experiencing suicidal and homicidal thoughts. I blamed the hospital, doctors, and even my parents for my suffering.
High school marked a turning point. I began counseling to process my trauma, develop healthy coping mechanisms, and address my anger. I learned to stop blaming my GI specialist and parents and realized the lengths they went to care for me. The first time I hugged my GI specialist, she cried—despite my earlier resentment, she had always fought for the best possible care. PTSD triggers still affect me with panic attacks, nightmares, and depressive episodes, but I am now equipped to seek help when needed.

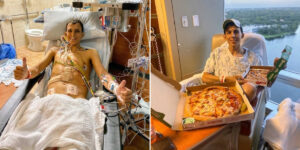
At age 15, I underwent ostomy reversal at a new hospital with a different surgeon. Complications followed: chronic vomiting, diarrhea, dehydration, and electrolyte imbalance required frequent hospitalizations and IV treatments. A small intestine ulcer eventually perforated, necessitating months of TPN and hyperbaric therapy. I bonded with hospital staff, who provided comfort during grueling treatments. During this period, I instinctively understood the severity of my condition and said my goodbyes to my mother, fearing I might not survive. Extensive testing finally led to exploratory surgery, which revealed adhesions creating a stricture that required removal.

My experiences at this hospital were markedly different from the children’s hospital. I received compassionate, personalized care throughout high school and college. My GI specialist pre-admitted me to avoid ER waits, requested pediatric floors for my care, and coordinated trusted anesthesiologists for my procedures. Nurses recognized me immediately upon admission and went out of their way to support me, even helping with basic tasks like washing my hair when I couldn’t shower. Small gestures like this helped me manage fear and anxiety.
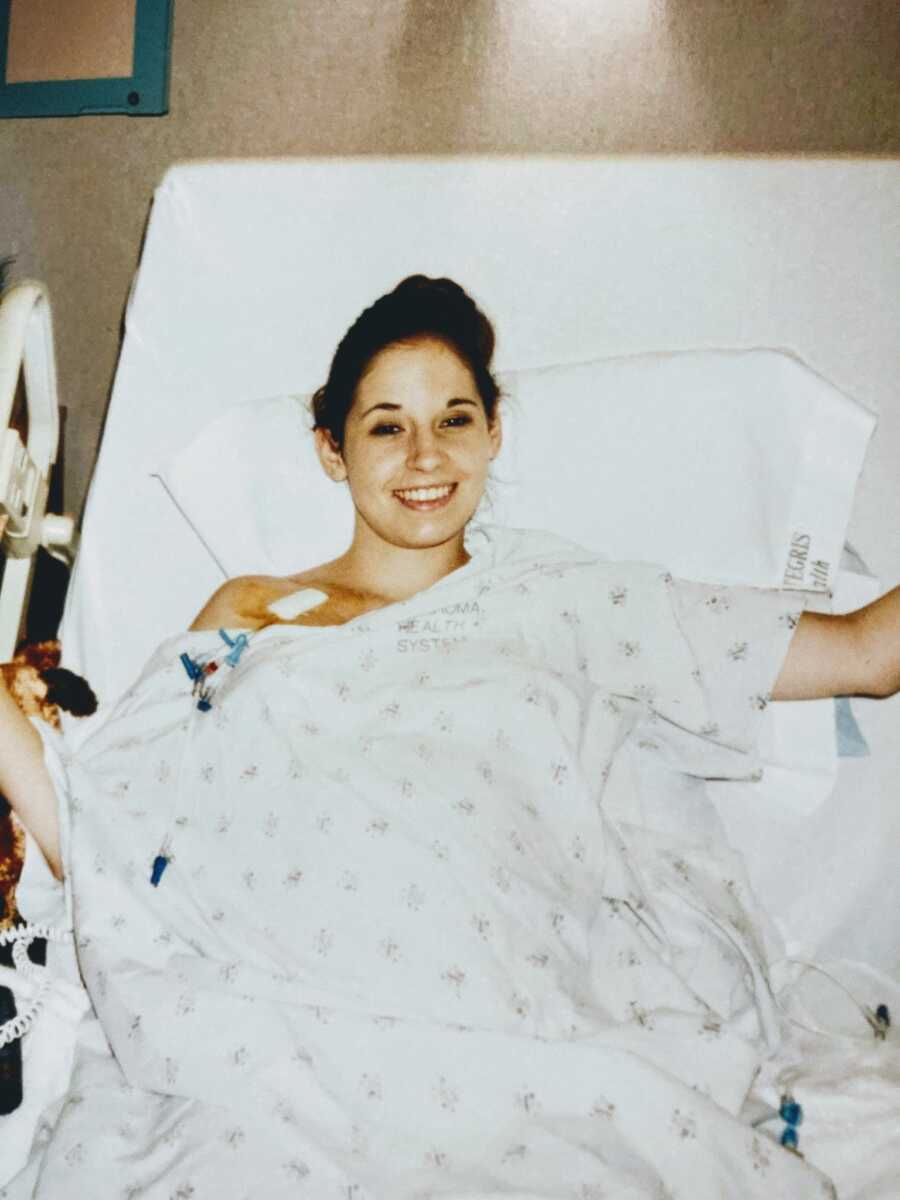
Despite chronic illness, I graduated high school on time and went on to earn a master’s degree. Teachers and professors accommodated my medical needs, providing tutoring and flexible learning arrangements during hospitalizations. My health has stabilized since college, allowing me to maintain full-time employment with a supportive employer.

I now dedicate my life to raising awareness about FAP and SBS through my blog, Life’s a Polyp, YouTube, social media, and Life’s a Polyp Shop, which features designs highlighting rare diseases and chronic illness. I am also publishing a children’s book about FAP, to be released on Rare Disease Day 2022. In 2015, I founded the NORD FAP Research Fund and donate all profits from my shop and a portion of my book sales to support FAP research. My journey has been fraught with challenges, but it has also shaped my passion for advocacy, resilience, and hope for others facing rare diseases.